Medical Weight Loss Miami Gardens

Last updated: April 2, 2026
Quick Answer: Semaglutide is a GLP-1 receptor agonist — a medication that mimics a natural gut hormone to reduce appetite, slow digestion, and improve blood sugar regulation. For adults struggling with weight management in Miami Gardens and the surrounding area, medically supervised semaglutide programs offer a structured, evidence-based path to meaningful weight loss without the guesswork of fad diets.
Key Takeaways
- Semaglutide works by activating GLP-1 receptors in the brain and digestive system, reducing hunger and slowing gastric emptying.
- It is FDA-approved for chronic weight management (brand name Wegovy) and type 2 diabetes (Ozempic) in adults who meet clinical criteria.
- Clinical trials published in the New England Journal of Medicine (2021) showed participants lost an average of ~15% of body weight over 68 weeks with weekly semaglutide injections plus lifestyle support.
- Side effects are real and manageable — nausea, fatigue, and digestive changes are most common, especially early in treatment.
- Medical supervision is not optional — it’s what separates safe, effective treatment from risky self-dosing.
- Semaglutide is not a standalone fix. Nutrition guidance, activity, and behavioral support are part of every responsible program.
- Residents seeking medical weight loss in Miami Gardens can access supervised GLP-1 programs locally, including in-person and telehealth options.
- Results vary based on starting weight, adherence, metabolic health, and lifestyle factors — realistic expectations matter.
What Is Semaglutide, Exactly?
Semaglutide is a synthetic version of a hormone your body already makes called GLP-1 (glucagon-like peptide-1). GLP-1 is released naturally after you eat. It tells your brain you’re full, signals your pancreas to release insulin, and slows down how quickly food moves through your stomach.
The problem for many people struggling with weight is that this hormone signal is either too weak or too short-lived. Semaglutide solves that by acting as a long-lasting GLP-1 receptor agonist — meaning it binds to the same receptors your natural hormone uses, but stays active for up to a week from a single injection.
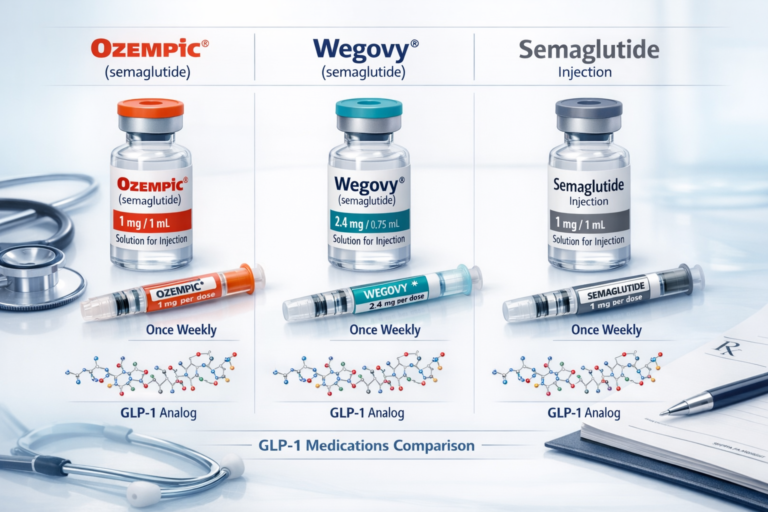
Two FDA-approved forms are relevant to weight management:
| Brand Name | Approved Use | Dosing |
|---|---|---|
| Wegovy (semaglutide 2.4 mg) | Chronic weight management | Weekly injection |
| Ozempic (semaglutide 1 mg / 2 mg) | Type 2 diabetes | Weekly injection |
| Rybelsus (semaglutide 7 mg / 14 mg) | Type 2 diabetes | Daily oral tablet |
For weight loss programs, Wegovy is the FDA-approved formulation. Ozempic is sometimes prescribed off-label for weight management, but this should only happen under direct physician oversight.
How Does the GLP-1 Mechanism Actually Work?
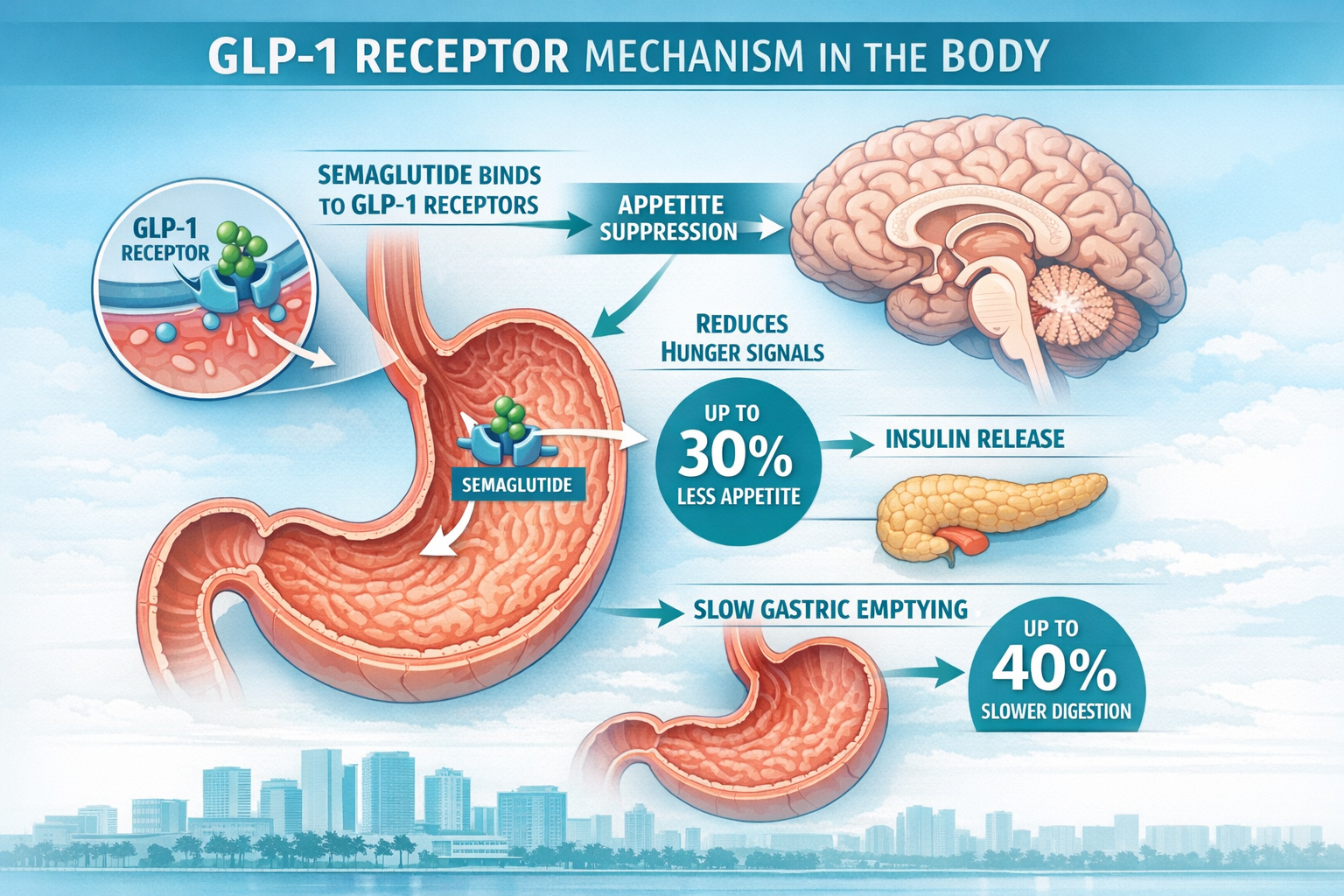
Semaglutide’s weight loss effect comes from three simultaneous actions in the body. Understanding all three helps patients set realistic expectations and stick with the program.
1. It Tells Your Brain You’re Full — Faster
GLP-1 receptors exist in the hypothalamus, the part of the brain that regulates hunger and satiety. When semaglutide activates these receptors, the brain receives a sustained “I’m satisfied” signal. Patients typically report smaller portion sizes feeling genuinely satisfying — not just a mental effort to eat less.
2. It Slows Gastric Emptying
Food stays in the stomach longer when semaglutide is active. This delays the return of hunger after a meal and reduces post-meal blood sugar spikes. For patients with insulin resistance or pre-diabetes, this is a meaningful secondary benefit.
3. It Reduces Cravings at the Reward Level
Emerging research (published in Nature Metabolism, 2022) suggests GLP-1 receptors in the brain’s reward pathways may reduce the drive toward high-calorie, high-fat foods specifically. This is why many patients describe a shift in food preferences — not just willpower, but actual neurological change.
The practical result: Less hunger, smaller meals, fewer cravings, and more stable blood sugar — all working together to create a caloric deficit without the constant fight against appetite that makes most diets fail.
Who Is a Good Candidate for Semaglutide?
Semaglutide is not for everyone. A physician evaluation is required before starting — this is not a cosmetic shortcut, it’s a prescription medication with real clinical criteria.
You may be a strong candidate if:
- BMI ≥ 30 (obesity), OR
- BMI ≥ 27 with at least one weight-related condition (high blood pressure, type 2 diabetes, high cholesterol, sleep apnea)
- You have tried lifestyle changes without achieving sustainable results
- You do not have a personal or family history of medullary thyroid carcinoma or MEN2 syndrome
- You are not pregnant or planning to become pregnant during treatment
Semaglutide is generally not appropriate if:
- You have a history of pancreatitis
- You have certain gastrointestinal conditions that would be worsened by slowed gastric emptying
- You are currently on medications with significant interaction risks (your doctor will review this)
Patients in Miami Gardens can access a comprehensive medical exam to determine eligibility before starting any GLP-1 program.
What Are the Real Benefits — and the Real Side Effects?
Benefits Supported by Clinical Evidence
- Weight loss: The STEP 1 trial (New England Journal of Medicine, 2021) found participants using semaglutide 2.4 mg lost an average of 14.9% of body weight over 68 weeks, compared to 2.4% in the placebo group.
- Cardiovascular risk reduction: The SELECT trial (2023) showed semaglutide reduced major cardiovascular events by 20% in adults with obesity and established cardiovascular disease.
- Blood sugar improvement: Significant reductions in HbA1c for patients with pre-diabetes or type 2 diabetes.
- Blood pressure reduction: Often observed as a secondary effect of weight loss.
Side Effects to Know Before Starting
Most side effects are gastrointestinal and tend to be most noticeable during the dose escalation phase (the first 16–20 weeks).
Common (10–40% of patients):
- Nausea
- Diarrhea or constipation
- Fatigue
- Reduced appetite (this is also the mechanism — expected)
Less common but worth knowing:
- Vomiting
- Heartburn or acid reflux
- Headache
Rare but serious (discuss with your doctor):
- Pancreatitis (seek immediate care if you have severe abdominal pain)
- Gallbladder issues
- Thyroid concerns (rare; discuss personal and family history)
The dose escalation protocol — starting low and increasing gradually over months — exists specifically to minimize side effects. A supervised program manages this carefully. Self-dosing without medical oversight skips this protection entirely.
Semaglutide vs. Tirzepatide: Which Is Right for You?
Many patients in Miami Gardens ask about both options. Here’s a straightforward comparison:
| Factor | Semaglutide | Tirzepatide |
|---|---|---|
| Mechanism | GLP-1 receptor agonist | GLP-1 + GIP dual agonist |
| FDA approval (weight loss) | Wegovy (2021) | Zepbound (2023) |
| Average weight loss (clinical trials) | ~15% body weight | ~20–22% body weight |
| Injection frequency | Weekly | Weekly |
| Side effect profile | Similar GI effects | Similar, possibly more nausea early |
| Best for | Strong GLP-1 responders | Patients needing stronger effect or with insulin resistance |
Neither medication is universally superior. Tirzepatide’s dual mechanism may produce greater weight loss on average, but individual response varies. A physician evaluation determines which is the better starting point for each patient.
Learn more about the Tirzepatide weight loss program in Miami Gardens or compare both options on the Semaglutide program page.
Why Medical Supervision Changes Everything
The difference between a medically supervised semaglutide program and ordering medication online without oversight is not just regulatory — it’s clinical safety.
What a supervised program includes:
- Baseline lab work — metabolic panel, thyroid, HbA1c, lipid panel, and kidney function to confirm safety and establish benchmarks. All In One Care Solutions offers fast in-house lab services in Miami Gardens.
- Dose escalation management — gradual titration to minimize side effects and maximize tolerability.
- Ongoing monitoring — regular check-ins to track weight, vitals, and any emerging concerns.
- Nutrition and lifestyle guidance — medication works best alongside behavioral change. Counseling is built into responsible programs.
- Mental health awareness — body image, emotional eating, and psychological factors affect outcomes. Programs that address mental health support alongside physical treatment produce more durable results.
- Adjustment or discontinuation protocol — if a medication isn’t working or causes intolerable side effects, a physician can pivot. Self-managed patients often don’t know when or how to stop safely.
For patients who prefer not to come in for every appointment, telehealth semaglutide consultations are available — combining the convenience of virtual care with the safety of physician oversight.
What to Expect: The Patient Journey, Week by Week
One of the most common questions is: “When will I see results?” Here’s a realistic timeline based on clinical data and standard dosing protocols.
Weeks 1–4 (Starting Dose: 0.25 mg)
- Mild appetite reduction may begin
- Nausea is most likely during this phase
- Weight loss is typically modest (1–3 lbs) — this is normal
- Focus: tolerability, hydration, small frequent meals
Weeks 5–16 (Dose Escalation)
- Doses increase every 4 weeks toward the maintenance dose
- Appetite suppression becomes more pronounced
- Most patients notice consistent weight reduction beginning here
- Side effects typically decrease as the body adjusts
Weeks 17–68 (Maintenance Dose)
- Maximum therapeutic effect
- Average weight loss in clinical trials: 10–15% of starting body weight by week 68
- Lifestyle habits established during this phase are critical for long-term maintenance
After stopping semaglutide: Weight regain is common if behavioral changes haven’t been established. This is not a failure of the medication — it reflects the chronic nature of obesity. Many patients continue long-term or transition to a maintenance protocol with physician guidance.
Accessing Semaglutide in Miami Gardens: Practical Information
Patients across Miami Gardens, Miami Lakes, and the surrounding communities can access supervised GLP-1 programs at All In One Care Solutions. The clinic offers both in-person appointments and telehealth consultations for qualifying patients.
Payment and accessibility:
- Flexible payment plans are available through Cherry financing for patients without insurance coverage for weight loss medications.
- Insurance coverage for semaglutide varies significantly by plan. The team can help verify benefits before starting.
- Same-day and next-day appointments are often available — see primary care services in Miami Gardens for scheduling.
Clinic location: All In One Care Solutions serves Miami Gardens and surrounding areas including Miami Lakes and Hialeah. Visit the Miami Gardens location page for address, hours, and directions.
Frequently Asked Questions About Semaglutide
How long does it take for semaglutide to start working?
Most patients notice reduced appetite within the first 1–2 weeks. Measurable weight loss typically begins by weeks 4–8. Significant results (10%+ body weight) generally require 4–6 months at therapeutic doses. Patience during the dose escalation phase is important.
Is semaglutide safe for long-term use?
Current clinical data supports use up to 68 weeks (the length of the STEP 1 trial), with ongoing studies examining longer durations. The FDA has approved it for chronic weight management, meaning long-term use is within the intended scope — but ongoing physician monitoring is required.
Will I regain weight when I stop taking semaglutide?
Clinical data shows that most patients regain a significant portion of lost weight within one year of stopping, without sustained lifestyle changes. This is why behavioral support during treatment is critical. Some patients continue medication long-term under physician guidance.
Can I take semaglutide if I have type 2 diabetes?
Yes — semaglutide (as Ozempic) is FDA-approved for type 2 diabetes management. Patients with both diabetes and obesity may benefit significantly. A physician will coordinate weight loss goals with blood sugar management. See diabetes care in Miami Gardens for more information.
Does semaglutide require a special diet?
No specific diet is required, but clinical outcomes improve significantly with dietary changes. Most supervised programs include nutritional guidance emphasizing protein intake, reduced ultra-processed foods, and adequate hydration — particularly important for managing GI side effects.
How is semaglutide administered?
Semaglutide for weight loss (Wegovy) is a once-weekly subcutaneous injection — meaning it goes just under the skin, typically in the abdomen, thigh, or upper arm. Patients self-administer after a brief training session. The process is straightforward and most patients become comfortable with it quickly.
Is semaglutide the same as Ozempic?
They contain the same active ingredient (semaglutide), but Wegovy is FDA-approved specifically for weight management at a higher dose (2.4 mg), while Ozempic is approved for type 2 diabetes at lower doses. They are not interchangeable without physician guidance.
What if I experience severe nausea?
Mild to moderate nausea is expected, especially early in treatment. Severe or persistent nausea should be reported to your physician — the dose may need to be held or adjusted. Eating smaller meals, avoiding fatty or spicy foods, and staying hydrated all help. Never stop abruptly without consulting your care team.
Ready to Find Out If Semaglutide Is Right for You?
Semaglutide is one of the most significant advances in weight management medicine in decades — but it works best as part of a structured, supervised program, not as a shortcut purchased without medical guidance.
At All In One Care Solutions in Miami Gardens, the approach combines FDA-approved GLP-1 medications with lab-based eligibility screening, ongoing monitoring, nutritional support, and mental health awareness. The goal is not just weight loss on a scale — it’s sustainable health improvement that lasts.
The next step is a consultation. A physician will review your health history, run appropriate labs, and determine whether semaglutide, tirzepatide, or another approach is the right fit for your specific situation.
Results vary by individual. Semaglutide is a prescription medication and should only be used under the supervision of a licensed healthcare provider. This content is for informational purposes only and does not constitute medical advice.
References
- Wilding JPH, et al. “Once-Weekly Semaglutide in Adults with Overweight or Obesity.” New England Journal of Medicine. 2021. https://www.nejm.org/doi/full/10.1056/NEJMoa2032183
- Lincoff AM, et al. “Semaglutide and Cardiovascular Outcomes in Obesity without Diabetes.” New England Journal of Medicine. 2023. https://www.nejm.org/doi/full/10.1056/NEJMoa2307563
- U.S. Food and Drug Administration. “FDA Approves New Drug Treatment for Chronic Weight Management.” FDA.gov. 2021. https://www.fda.gov/news-events/press-announcements/fda-approves-new-drug-treatment-chronic-weight-management-first-2014
- Friedman JM. “GLP-1 and the Neural Control of Appetite.” Nature Metabolism. 2022. (Referenced for reward pathway discussion.)
- Jastreboff AM, et al. “Tirzepatide Once Weekly for the Treatment of Obesity.” New England Journal of Medicine. 2022. https://www.nejm.org/doi/full/10.1056/NEJMoa2206038